Father Time: Aortic Dissection Style
You have heard the expression “Father Time”.
This edition of Aortic Academy at BadAorta.com will discuss the timing of treatment and intervention for acute Type B Aortic Dissections.
Many people with aortic dissections are focused on what treatment options are available to them, but few actually consider that timing of the treatment can also be an important variable to consider.
It has also been shown that TEVAR for a certain subset of acute Type B aortic dissections are beneficial.
Timing is Everything - Sort Of
When we are discussing “timing” of intervention for Type B Aortic Dissections, we define “time” as the interval between initial presentation of the aortic dissection to the current time point. For example, if someone developed a new aortic dissection on January 1, 2018 then that is the starting time point. If January 14, 2018 would be an interval of two weeks, etc.
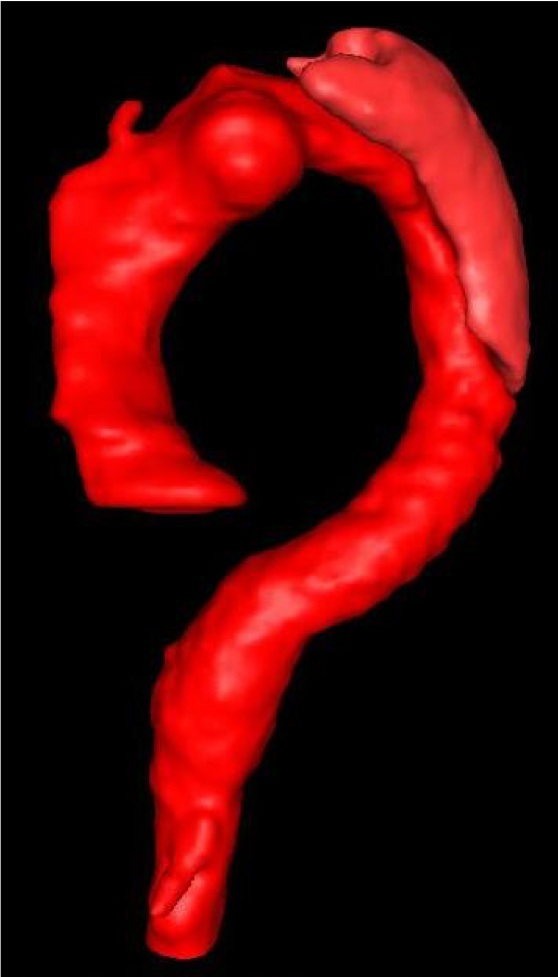 Acute Type A aortic dissections should be treated immediately upon diagnosis and without delay. The treatment is open heart surgery.
Acute Type A aortic dissections should be treated immediately upon diagnosis and without delay. The treatment is open heart surgery.
For uncomplicated Type B aortic dissections - those aortic dissections where there is no malperfusion, impending rupture or uncontrolled hypertension - there is an art and science about when to intervene with TEVAR (Thoracic Endovascular Aortic Repair).
The initial management for uncomplicated Type B aortic dissections is to immediately control the patient’s blood pressure.
The patient’s blood pressure should be controlled and ideally range in the systolic range from 100 mmHg to 125mmHg. Frequently, intravenous (IV) antihypertensive medications are initiated because of the rapid onset of action associated with intravenous administration as compared to oral medications (pills).
Antihypertensive medications such as lopressor, esmolol and labetalol are the first line agents and are classified as beta-blockers, which decrease the pulse pressure on the aortic wall and reduces the strain on the fragile acute aortic dissection.
Once the blood pressure is controlled, there is now time to re-evaluate the situation.
Acute, uncomplicated Type B aortic dissections are classified as acute, subacute or chronic based on the time interval between the original presentation, or start of the aortic dissection, and the current assessment period.
- Acute phase: 0 - 14 days after presentation
- Subacute phase: 15 - 90 days after presentation
- Chronic phase: greater than 90 days
It is common to repeat a computed tomography (CT) scan of the aortic dissection several days after initial presentation to the hospital and the initial CT Scan performed in the emergency room.
On occasion, it is necessary to perform several CT scans during the hospitalization to confirm that there are no new changes to the aortic dissection flap and aorta. These scans are done every few days and are the most effective way to ascertain if the aortic dissection is stable radiographically or if it is slowly changing or evolving.
A small fraction of patients with acute Type B aortic dissections will continue to experience an extension of the original tear after the initial presentation. Sometimes there are no indications that there is a continued tearing of the aorta except as seen on CT scan.
If there is continued tearing (dissection) of the aorta on CT scan after the initial presentation and with continued blood pressure control, then the uncomplicated Type B aortic dissections becomes “complicated” and intervention with TEVAR is indicated during the acute phase (0-14 days).
After there is radiographic confirmation that the aortic dissection has not evolved or changed or continued to dissect, then it is ideal to transition from intravenous blood pressure medications to oral hypertensive medications in preparation to discharging the patient home.
Evolution of Our Thinking on Type B Aortic Dissections
Our thinking on the optimal timing for intervention with TEVAR in patients with uncomplicated Type B aortic dissections has evolved.
We used to intervene in the acute phase during the initial hospitalization, but found that TEVAR interventions in the subacute phase were safer for the patients.
Currently, we discharge stable patients home with optimal blood pressure control on oral antihypertensive medications. We see them back in 2-3 weeks in the office to assess their symptoms and blood pressure control. We also obtain another current CT scan to assess the aortic dissection and aortic dimensions.
We then discuss performing a TEVAR procedure within the next several weeks, in the subacute aortic dissection phase and prior to the chronic aortic dissection phase.
Factors Involved in Treating Type B Aortic Dissections
There are many potential factors on why TEVAR in the subacute aortic dissection phase is safer.
Primarily, the safety for intervening in the subacute phase relates to the stability of the aortic dissection flap and associated lining of the aortic wall called the intima.
In the acute phase, when the aortic dissection is “fresh”, the flimsy flap of tissue inside the lumen of the aorta called the aortic septum has the consistency of wet tissue paper.
 In addition, the lining of the aorta that is not affected by the dissection flap is also fragile and more pre-disposed to extending the aortic dissection.
In addition, the lining of the aorta that is not affected by the dissection flap is also fragile and more pre-disposed to extending the aortic dissection.
One analogy to better understand this is an earthquake fault line. When an earthquake occurs, there is a pre-existing fault line that suddenly shifts. When the earthquake happens, the fault line is worsened and the separation in the earth is widened.
Furthermore, after the initial earthquake, there can be after shocks. These after shocks can also can damage and affect the integrity of the fault line and even create new tears in the earth’s crust.
Aortic dissections occur suddenly along pre-existing invisible fault lines that develop in the lining of the aorta over time.
When the aortic dissection occurs, the fault lines are expanded and the aortic wall separates.
Within the first two weeks of the initial dissection, the equivalent of after shocks can happen which can extend the dissection. Poorly controlled blood pressure following an aortic dissection can increase the chances that the dissection could extend.
This is why it is so critical to optimally control the blood pressure in the acute phase.
In the chronic phase of the aortic dissection, optimal blood pressure control is important to minimize the risk of progressive aortic dilation of the false lumen over time which could lead to an aortic aneurysm years later.
The body’s natural inclination after an aortic dissection is to begin to heal the torn tissues that the process stabilizes.
The newly torn tissues (aortic dissection flap or aortic septum) begin to thicken up with scar tissue. The body recruits fibroblasts into the tissues to give them more integrity.
The more integrity that the aortic dissection gains, the less chance that another dissection could occur.
By waiting two weeks (minimum) and intervening with TEVAR in the subacute phase, we take advantage of the healing that is going on within the tissues of the aortic wall.
Therefore, the TEVAR in the subacute phase is less likely to create a new tear, extend the current tear or traumatize the aortic tissues which could complicate the procedure.
Summary
In summary, aortic dissections are complex problems that require well-thought care patterns.
Optimal blood pressure control is the bedrock of management of uncomplicated Type B aortic dissections.
TEVAR for Type B aortic dissections is recommended in the subacute phase of the dissection to minimize the chances of disturbing the fragile aortic dissection tissues during the TEVAR procedures which could complicate the situation and compromise the effectiveness of the TEVAR therapy.
Was this post informative?
Subscribe to my newsletter to learn more about the aorta, its diseases, and how to treat them.
Comments
Share your thoughts below — I try to get back to as many comments as possible.